The Complement System
Part 3 of the Innate Immune System Review.
Introduction
Series Recap:
Welcome to part 3 of the innate immune system review. Part 1, The Innate Immune System, introduced its core components, including phagocytic cells, the initiation of inflammation, and the complement system. This foundational overview set the stage for understanding the body’s frontline defense against pathogens. Part 2, Inflammation: It’s not Just Swelling, took a deeper dive into the process of inflammation. Part 2 also explored the biomarkers and their assays that help to diagnose acute and chronic inflammation. Part 3, The Complement System, explores how complement interacts with both the innate immune system and the inflammatory response. This article will also review the process of testing the function and presence of the complement system.
Purpose & Overview
1. Goal: explore complement system and provide an in-depth look as lab test methods and implications
2. Highlight the need for complement testing for diagnosis and management.
The Complement System: An Overview
Historical and Biological Significance:
Intonations of the complement system were first noticed in the late nineteenth century as scientists began to notice that serum possessed bactericidal attributes. Because of its complexity, multiple scientists made ‘complementary’ discoveries that together shaped early the early understanding of the complement system. These scientists included Buchner and colleagues, Jules Bordet, and Paul Erlich. Erlich pioneered the idea that complement functioned alongside antibodies to kill bacteria. By the mid-twentieth century, all component proteins and pathways as we know today were ironed out. (2)
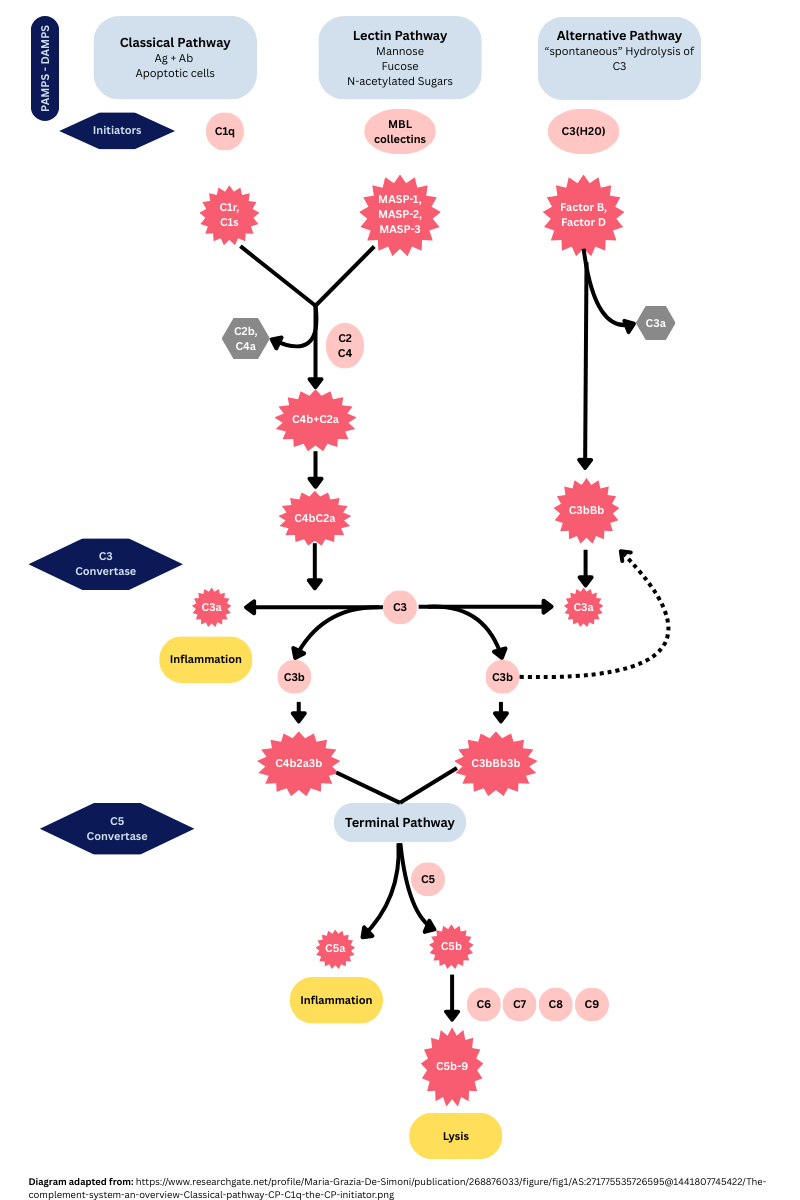
Complement, often referred to as a cascade, is composed of enzymatic proteins called zymogens. (1) Similar to the coagulation cascade (click here for more information), each activated protein becomes the activating enzyme for the next protein in the cascade. (1) Complement proteins interact to kill bacteria and promote inflammation. (1) There are three pathways complement is executed based on the initiator: classical, alternative, and lectin pathways. (2) The classical pathway is activated when C1 protein either binds with antibodies attached to the bacterial cell surface or directly to the bacterial surface. (1) The alternative pathway begins with the spontaneous hydrolysis of C3 protein. (1) This pathway also provides positive feedback, ramping up the activity of the classic and lectin pathways. Finally, the lectin pathway begins when collectins (multimeric lectin complexes) bind to mannose, a sugar present only on bacteria. (2) To a lesser extent, several coagulation factors can initiate the complement system. These include factors Xa, XIa, VIII, and plasmin. (2) All three pathways converge to the activation of C3 and the formation of pores (membrane attack complex - MAC) on the bacterial cell surface. This weakens the bacteria by allowing the internals to be extruded. See figure 1 depicting the mechanics of the various pathways.
Figure 1
Role in Innate Immunity:
Complement strengthens innate immunity through three key functions: (1)
1. It binds to pathogens, opsonizing them for phagocytosis.
2. Fragments leftover from complement activation recruit and activate phagocytes.
3. Terminal complement components form large pores on bacterial membranes, leading to cell lysis.
Activated complement proteins, specifically C5a and C3a, promote local inflammation. (1) C5a dominates this function due to the ubiquitous presence of C5a receptors on inflammatory cells, such as dendritic cells, and non-inflammatory cells. (2) The following actions reflect C5a’s ability to promote inflammation: (2)
· Promotes neutrophil mobility and aggregation.
· Promotes release of inflammatory cytokines and lysozymes by monocytes and macrophages.
· Improves adhesion between neutrophils and endothelial cells.
C3a promotes inflammation to a lesser extent. It promotes eosinophil and mast cell migration. (2)
Relevance to Disease:
Diseases linked to complement span two basic categories:
1. Deficiencies of one or more complement proteins.
2. Dysregulation of the complement cascade.
Deficiencies can be inherited or acquired. Genetic deficiencies follow a recessive inheritance pattern, requiring both parents to carry the affected gene. Acquired deficiencies occur when protein synthesis malfunctions (such as in liver disease), protein loss (such as in severe burns), overconsumption, or autoimmunity against complement components. Either inherited or acquired deficiencies result in recurrent infections and pyogenic infections, especially infections of Neisseria species. (3)
Dysregulation is commonly encountered in many autoimmune diseases and direct damage to the kidneys. Complement contributes to excessive tissue damage in lupus erythematosus, vasculitides, Sjogren’s syndrome, antiphospholipid syndrome, systemic sclerosis, dermatomyositis vasculitides, and rheumatoid arthritis. (4) The kidneys are often the target of unregulated complement, resulting in atypical hemolytic uremic syndrome, C3 glomerulopathy, and paroxysmal nocturnal hemoglobinuria. (5)
Lab Testing
Why Test Complement
Complement testing is not always an immediate consideration, but it can help solve complex medical cases. The best reason to test for complement is to discover the “why” behind recurrent infections and explore the inflammation and damage associated with autoimmune diseases. Once a clinician knows the “why”, targeted therapeutics are deployed to help treat a disease.
Objectives of Testing:
1. Establish the functionality by exploring qualitative and quantitative aspects of the complement cascade.
2. Assist in tailoring effective treatments for patients.